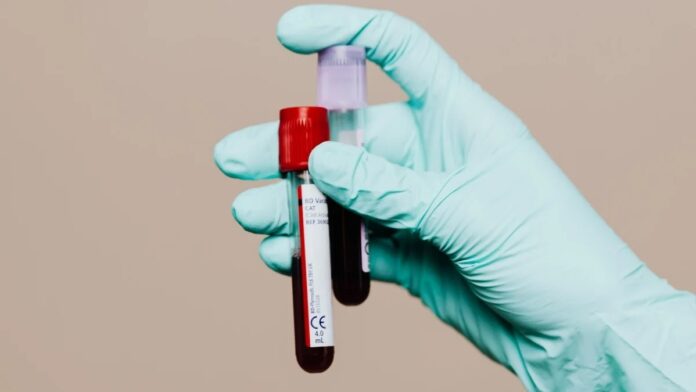
A breakthrough in neurological diagnostics may soon allow doctors to identify the earliest signs of Alzheimer’s disease through a simple blood test, potentially years before traditional imaging methods can detect brain changes.
New research led by Mass General Brigham suggests that a specific blood biomarker, known as pTau217, serves as a highly accurate early warning system for the protein accumulations that drive Alzheimer’s progression.
The Science Behind the Breakthrough
Alzheimer’s disease is characterized by the toxic buildup of two proteins in the brain: amyloid-beta and tau. For years, the gold standard for detecting these “clumps” and “tangles” has been Positron Emission Tomography (PET) brain scans. While effective, PET scans are expensive, invasive, and typically only show abnormalities once significant damage has already begun.
The study reveals that the pTau217 biomarker operates on a much earlier timeline:
– Earlier Detection: pTau217 can identify high-risk individuals even when their PET scans appear completely normal.
– Predictive Power: High levels of the biomarker are closely linked to future protein accumulation, while low levels suggest a minimal risk of developing the disease in the near term.
– Cognitive Correlation: Higher concentrations of pTau217 were linked to a greater likelihood of cognitive decline, particularly in patients already showing early signs of amyloid-beta buildup.
How the Study Was Conducted
To validate these findings, researchers tracked 317 cognitively healthy participants (aged 50 to 90) over an average period of eight years. By combining data from blood tests, PET scans, and cognitive assessments, the team was able to map how blood chemistry changes in relation to physical brain pathology over time.
“We used to think that PET scan detection was the earliest sign of Alzheimer’s disease progression… But now we are seeing that pTau217 can be detected years earlier, well before clear abnormalities appear on amyloid PET scans.”
— Hyun-Sik Yang, Neurologist at Mass General Brigham
Why This Matters for the Future of Medicine
This discovery represents a significant shift in how we approach neurodegenerative diseases. Traditionally, Alzheimer’s diagnosis has been reactive—identifying the disease after cognitive symptoms emerge. Moving toward a proactive model through blood testing could change the landscape of treatment in several ways:
- Early Intervention: Detecting risk decades in advance could allow for lifestyle interventions or new drug therapies to be administered before irreversible brain damage occurs.
- Clinical Efficiency: Blood tests are significantly more accessible, affordable, and less invasive than PET scans, making large-scale screening more feasible.
- Research Acceleration: Identifying high-risk individuals earlier allows pharmaceutical researchers to test new drugs on patients in the very earliest stages of the disease.
Challenges and Next Steps
Despite the promise, the transition from the lab to the doctor’s office is not immediate. The research team noted several hurdles that must be cleared:
– Data Diversity: Larger and more diverse study groups are required to refine the prediction algorithms and ensure accuracy across different populations.
– The “Dementia Gap”: While the test can predict protein buildup, scientists must still determine how accurately these biological changes translate into actual dementia symptoms, as not everyone with protein accumulation develops full-scale cognitive impairment.
Conclusion
By identifying the biological precursors of Alzheimer’s long before they appear on a brain scan, the pTau217 blood test offers a vital opportunity to “push back the clock,” potentially transforming Alzheimer’s from an inevitable decline into a manageable or preventable condition.